Meniscus Diagnosis
Meniscal injuries can be detrimental to an athletic career, can severely impair a patient’s quality of life, or can be an asymptomatic finding that can resolve without surgery. Understanding the type of injury and the healing potential of the injury are critical to determining when surgery is needed and when it is not. When a patient visits Dr. Chahla, there are several aspects of the diagnostic process that provide him with critical information to generate optimal patient specific treatment plans.
History and Physical Exam
The first is a patient’s history, which is, simply put, who they are, what happened, how it happened, when it happened, and what they expect. This allows us to understand the cause of the injury as well as characteristics about the patient’s lifestyle, goals, and health. The next step is a physical exam. The physical exam allows us to pinpoint the exact cause of an injury and helps us determine what imaging would be best for a given patient. Two common exam maneuvers are the McMurray Test and the Apley’s compression test. These maneuvers test for meniscal injury by eliciting pain upon a twisting/rotating motion of the knee.
Imaging
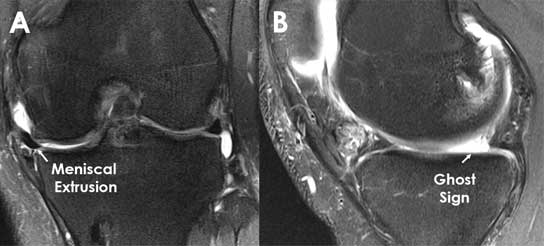
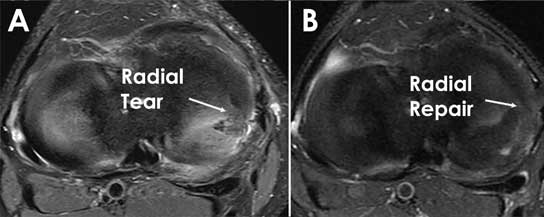
For imaging, x-rays are a standard for all patients. While the meniscus cannot be adequately assessed on an x-ray, it helps Dr. Chahla to see the entire joint and any other potential issues that could either contribute to symptoms or affect recovery. If the combination of your history, physical exam, and x-ray suggests a meniscal injury, the next best step would be an MRI (magnetic resonance imaging). This uses powerful magnets to create detailed snapshots of your bones, cartilage, ligaments, and other soft tissues.
Arthroscopy
For certain surgical cases, we cannot decide the best treatment plan until we directly look at the meniscus. This is done with an arthroscope (camera) in the operating room after the patient has been sedated with anesthesia. In this scenario, we will go into the operating room with two plans for a patient. Preoperatively, the patient will be aware of both options, understand the risks/benefits of each option, and provide consent for both procedures. When Dr. Chahla can directly see the meniscus and the surrounding joint with the arthroscope, he will decide the better of the two treatment plans based on these findings, the patient’s specific history, and the patient’s specific goals.
Dr. Jorge Chahla offers cutting-edge procedures and treatment to help patients return to the lives they love after suffering complex injuries to the hip, knee, and shoulder. Contact Dr. Chahla to schedule a consultation today. Dr. Chahla has orthopedic clinics in Chicago, Naperville, Oak Brook, and Munster Indiana.
At a Glance
Dr. Jorge Chahla
- Triple fellowship-trained sports medicine surgeon
- Performs over 500 surgeries per year
- Assistant professor of orthopedic surgery at Rush University
- Learn more


