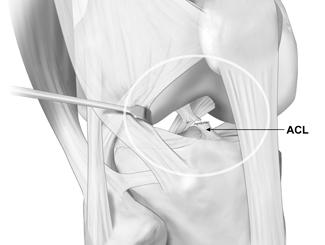
ACL Injuries
What are the symptoms of an ACL injury?
When you injure your ACL, you may hear or feel a “pop” at the time of injury coupled with buckling of the knee. There will be immediate and intense knee pain, swelling, inflammation, redness, and bruising. The pain may resolve, but the knee will likely remain unstable, especially when attempting to quickly pivot or change direction. Additionally, you may experience a loss of knee range of motion following an ACL injury. Finally, symptoms such as tenderness along the knee joint or locking of the knee if there is an associated meniscus tear that occurs. Continuing regular activities with a deficiency in your ACL may lead to additional instability episodes, which can cause more damage to other structures such as the meniscus and cartilage. If you feel that you may have suffered an injury to your ACL, it is important to have it evaluated by a well regarded knee surgeon, like Dr. Jorge Chahla, as soon as possible.
A torn anterior cruciate ligament (ACL) is a serious knee injury that can affect your ability to walk, run, or participate in sports. Whether caused by a sudden twist, direct impact, or a non-contact pivot, an ACL injury often leads to instability and persistent knee pain. Dr. Jorge Chahla, a leading orthopedic knee surgeon with offices in Chicago, Naperville, and Oak Brook, specializes in the diagnosis and treatment of ACL injuries. If you have experienced knee instability, swelling, or difficulty bearing weight, contact Dr. Chahla to discuss your treatment options and take the first step toward restoring your knee function.
- Triple fellowship-trained sports medicine surgeon
- Performs over 800 surgeries per year
- Associate professor of orthopedic surgery at Rush University
- Learn more