Meniscus Transplant
A meniscal transplant is a technically challenging procedure that is available to patients who have failed a prior meniscal repair and subsequently underwent a total meniscectomy or who simply had a prior total meniscectomy with an outside orthopedic knee surgeon. These patients are typically followed closely for the rapid development of osteoarthritis and are offered meniscal replacement to preserve their joint health. The goal of a meniscal transplant is to restore proper function and structure to a knee that has lost its native meniscus. This will allow for improved shock absorption within the knee and an improved fit between the bones of the knee.
It is typically indicated for younger patients who have undergone a total meniscectomy and continued to have symptoms that are affecting their quality of life or ability to perform the activities of daily living. These patients must fail to have adequate improvement with non-operative management before a meniscus transplant can be recommended. Patients with extensive cartilage damage are also poor candidates for the procedure as there will be difficulty in placing the transplanted meniscus due to the reduced joint space associated with an arthritic joint. Other typical drawbacks and limitations of a meniscal transplant are similar to transplants of other organs: there is always an inherent immunologic risk, a limited risk of disease transmission, and limited donor availability.
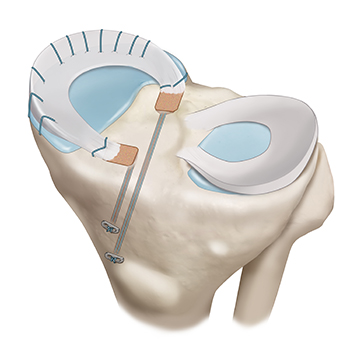
If a patient elects to proceed with a meniscal transplant, they will have preoperative imaging to allow for proper sizing. When a size matched and immunologically matched graft is available, the patient will be scheduled for surgery with Dr. Chahla. During the procedure, an incision is made alongside the patellar tendon to allow for insertion of the meniscal allograft. The meniscal graft can be secured using a variety of techniques including a bone plug technique and a bone fixation technique. Currently, there is no evidence to suggest one technique is superior to the other.
Among the rehabilitation regimens after a meniscal surgery, rehabilitation for a meniscal transplant is the strictest. The transplanted meniscus needs to be allowed a generous amount of time to integrate with the surrounding tissue. Failure to adhere to the strict rehabilitation regimen could lead to the ultimate failure of the surgical intervention. For the first 6 weeks, the patient is required to use a knee immobilizer and maintain a strict non-weight bearing with crutches. From 6-8 weeks, the patient will begin weight bearing and progress to full weight bearing. They will continue to have a restricted range of motion until 8 weeks. By 12 weeks, they can begin higher strain functional activities including lunges.
For patients who have lost a significant portion of their meniscus due to previous surgery or injury, meniscus transplant surgery may be a viable option. This procedure involves replacing the damaged meniscus with a donor graft to restore knee function and delay the progression of osteoarthritis. Leading orthopedic knee surgeon Dr. Jorge Chahla is an expert in meniscus transplantation, offering advanced solutions for patients seeking long-term knee preservation. If you are experiencing chronic knee pain following a previous meniscus surgery, schedule an appointment with Dr. Chahla in Chicago, Naperville, or Oak Brook to discuss whether a meniscus transplant is right for you.
At a Glance
Dr. Jorge Chahla
- Triple fellowship-trained sports medicine surgeon
- Performs over 800 surgeries per year
- Associate professor of orthopedic surgery at Rush University
- Learn more

